If you take insulin to manage your diabetes, you could be taking anywhere from 1 to 10 injections per day.
And where you inject your insulin matters — not only because certain areas of the body are more ideal than others, but also because it’s important to use a variety of areas.
In this article, we’ll discuss everything you need to know about insulin injection sites.

Table of Contents
- Why it matters where you inject your insulin
- What are the best injection sites for insulin?
- Why you should rotate your insulin injections
- How I rotate my insulin injection sites
- Lipodystrophy: a side-effect of not rotating injection sites
- Never inject two types of insulin in the same area at the same time
- Can you inject insulin into muscle?
- Proper and safe insulin injection technique
Why it matters where you inject your insulin
Insulin is designed to be injected (or delivered via an insulin pump) into body fat — also known as “subcutaneous tissue.”
The rate at which your insulin is absorbed is largely based on the assumption that it’s being injected into fat, rather than muscle.
When a pharmaceutical company tells you that the “onset” of your Novolog or Humalog insulin is 15 minutes, for example, that is based on when it is injected into body fat. The “peak” of its efficacy and the “duration” of it staying in your bloodstream also depends on it being injected into body fat — not muscle.
What are the best injection sites for insulin?
The best injection sites for insulin are a variety of locations on your body that are both easy to reach and contain adequate body fat. (The leaner you are, the more you may need to “pinch” your layer of fat in order to avoid injecting into muscle.
- Belly fat
- Side-torso fat (“love handle” area)
- Lower back fat
- Thigh fat (on the outer or inner sides of your leg)
- Butt fat (upper, middle, sides, etc.)
- Arm (back or sides)
These areas are the most likely to have enough body fat to comfortably inject insulin into using a pen or syringe.
UPDATE: I recorded this YouTube video to show you where I inject my insulin:
Why you should rotate your insulin injections
Every time you inject insulin into a certain area of your body, that location of skin and body fat is “injured” and has to heal. Over the course of years injecting insulin into your body, scar tissue will develop.
You may not see evidence of that scar tissue on the outside of your body, but it’s there on the inside.
The more you inject insulin into the back of your arm, the more scar tissue will develop there. As people with diabetes, it’s very easy to get into the habit of injecting into the same spot over and over because it’s easy to reach and comfortable to access in the middle of a restaurant, for example.
But scar tissue will significantly affect your body’s ability to absorb the insulin from that last injection, and you could end up needing more insulin to do the same job even though your insulin needs didn’t change. Instead, it’s just scar tissue built up and interfering with the absorption of your insulin dose.
Rotating your injection sites is critical.
- If you used your left arm for your lunchtime injection, you should use your right arm for your dinnertime injection.
- If you used the left side of your bum for your long-acting insulin injection last night, you should use your right side for tonight’s injection.
The more you can rotate the areas of your body and the exact spots on each area, the less scar tissue will build up and the more easily your body will absorb that insulin.
How I rotate my insulin injection sites
While I use my abdomen and arms for my rapid-acting injections, I use my glutes and lower back for all of my basal (long-acting insulin) injections.
I have a very homemade but also very effective way of keeping track of my injections so I remember to rotate them.
To make sure that I do proper injection rotation, I have a piece of paper where I note down my injections (see image below). I usually switch from right to left side daily and will start with injecting right above the bikini line, then switch to below the bikini line, and lastly inject alongside the bikini line.
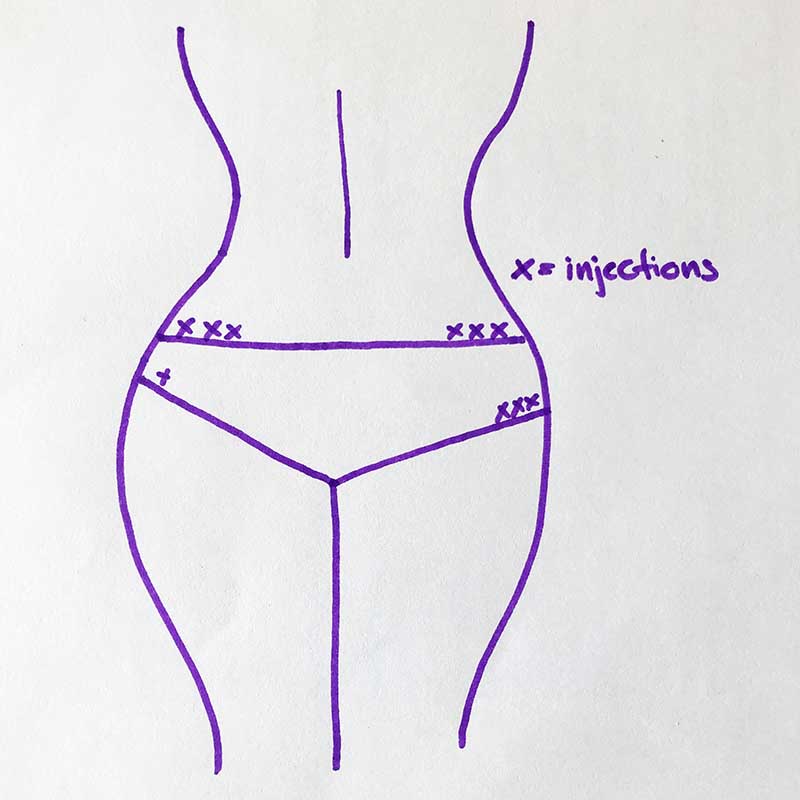
This rotation pattern takes me about a month to get through before I start all over again. So far, that has worked really well for me. I have no lumps and my insulin absorption is still really good after 20 years with diabetes.
Lipodystrophy: a side-effect of not rotating injection sites
Lipodystrophy (LD) is a condition affecting body fat tissue and it’s very common in people who take multiple daily insulin injections. Other variations include “lipohypertrophy” (LH) or “lipoatrophy” (LA). All of which concern damage, scar tissue, or hard lumps in the fatty tissue where you’ve been injecting insulin.
The best way to prevent LD from developing in your skin tissue is by making sure you rotate your injection sites and don’t repeatedly inject insulin into the same area of tissue.
If you already have signs of LD, you can talk to your primary care and ask for a referral to a dermatologist for further guidance on reducing it.
Never inject two types of insulin in the same area at the same time
You should also keep in mind that you do not want to inject two different types of insulin in the same area at the same time.
If you’re taking a long-acting insulin dose and a rapid-acting insulin dose at 7 a.m., you should make sure they are injected into two completely different areas of your body.
Some insulins can affect the potency, absorption, and efficacy of other insulins if they “meet” each other in that subcutaneous tissue.
Can you inject insulin into muscle?
The short answer is yes, but you shouldn’t inject insulin into muscle unless it’s very intentional and you understand the consequences and risks.
Injecting insulin directly into muscle is going to completely change how quickly it is absorbed into your bloodstream and how quickly it starts affecting your blood sugar levels.
The “onset,” “peak,” and “duration” will all change when insulin is injected directly into muscle tissue.
(It’s also going to be a bit more painful!)
Learn more: Injecting Insulin into Muscle: Do’s and Don’ts
Never inject long-acting insulin into muscle.
Long-acting insulin (Tresiba, Lantus, Toujeo, Basalgar, NPH, Levemir) needs to stay active in your body for the intended duration of time.
Injecting it into muscle means it’s going to be out of your bloodstream far sooner and thus put you at a high risk for severely high blood sugars and diabetic ketoacidosis (DKA).
Consider injecting rapid-acting insulin into muscle if…
When treating a high blood sugar with a correction dose of insulin, the amount of insulin you use needs to be finely tuned to ensure your blood sugar doesn’t severely plummet.
The goal is to bring your blood sugar back down into a safe range — that requires an accurate “correction factor” and some patience.
You can consider injecting insulin into muscle if:
- Your blood sugar is extremely high, over 250 mg/dL. Injecting your correction dose of insulin into muscle could help it come down sooner.
- Your insulin pump failed and you need to get insulin active in your system as quickly as possible.
- You’re combating sudden severe stress that is going to (or has already) spiked your blood sugar.
- You take steroids for a condition like Addison’s disease. Consider injecting the insulin dose you use to compensate for that steroid dose into muscle.
- Your blood sugar is high because you’re severely dehydrated and potentially producing ketones.
- Your blood sugar is high prior to an important activity that calls for a lower blood sugar level (like an athletic event or surgery).
- You forgot to take insulin with your meal. Injecting directly into muscle can help get the insulin on board sooner and prevent that post-meal spike.
Keep in mind that you should always talk to your doctor prior to making changes in how you take your insulin.
Proper and safe insulin injection technique
Well, this is simple. Every time you inject insulin into body fat or muscle, it’s important to ensure that the area is clean and that you are using a clean syringe or insulin pen.
Insulin syringes and pen needles are designed to be used once.
And you should sanitize the intended injection site with an alcohol swab before every injection.
Is this realistically always possible? Not really — not in the real life of diabetes when you’re taking many injections a day. But the goal is to inject insulin into the cleanest location possible to prevent infections.
Having to inject insulin into your body on a daily basis is not fun, but it keeps us alive. The more thought and consideration you put into where you inject your insulin, the better off you’ll be.




Sally Wheldon
Interesting article on injecting but I don’t understand HOW to inject into muscle, should I wish to do so. Please help.
Shahid mahmood
It’s good article. Really helpful to understand the concept of using insulin’s. Keep update to provide more useful tip to live healthy with Diabetics.
Jeo
Great guide! I’ve been injecting insulin for a while, and finding the right sites can make such a difference in comfort and absorption. I rotate between my abdomen, thighs, and upper arms, but I’ve definitely noticed some spots work better than others. Using proper rotation not only helps with absorption but also prevents lumps and bruising. Tips like these are really valuable for anyone managing diabetes it’s all about making injections as smooth and painless as possible!
Lori Izeman
How come some shots leave bruises?
Donna
I’m new at using insuline and it was explained very well
Karen Maccurdy Thompson
How could a dermatologist help with issues of LIpodystrophy?
Phil
Thank you very much for this. My husband injected Lantus into a stomach muscle I think last night and has a lump. Now he just injected into his upper thigh. Thank you! NP never educated us on the proper procedure other than into the abdomen.
Peter Brown
So, what about insulin pumps? I know I use the same place for 3-6 days. Any thoughts?
Christel Oerum, MS
You should rotate your site every time you change you cannula.
Medtronic has this suggestion:
Choose insertion sites and remember to rotate using these two methods: Visualize an imaginary clock drawn on your belly button. Rotate sites by starting at the 12 o’clock position and then rotating clockwise to 3, 6 o’clock, and so on. Imagine a capital M or W drawn on your body.
Shawna
Hello. I really appreciate all the helpful info you provide. New T1 here… looking at your picture, I can’t figure out how you fit 30-60 long acting insulin shots in your backside over a month. Can you share a picture of your drawing filled up showing where you put the rest of the shots? I’ve not tried my arm for yet. Do you not need to pinch skin first?
Christel Oerum
I made a YouTube video where I show it, hopefully, that helps (https://youtu.be/YryAsIqWNFA)
Bird
Hi – Thank you so much for this page! Until now, I have been able to manage my diabetes type 2 with just metformin and diet but when I was put on a cortisteroid 2 weeks ago I was given Basalgar and Novalog pens with little instructions. I learned more from 5 minutes reading this page than I have in two weeks of trying to figure everything out on my own! So helpful!
Christel Oerum
First off, I’m sorry you haven’t been given better instructions from your medical team but I’m glad we can be a resource. You might also find our YouTube helpful – https://youtu.be/AIhcpWBP_cQ