Thyroid disease and diabetes often go hand in hand, and it’s something you should keep an eye on since thyroid disease can significantly impact your diabetes and your overall well-being.
Key facts
- Hypothyroidism is when the thyroid gland is underactive and doesn’t produce enough hormones. Hyperthyroidism, on the other hand, occurs when the thyroid is overactive and produces too many hormones. Both conditions affect the body’s metabolism and can significantly impact overall health.
- In hypothyroidism, symptoms include unexplained weight gain, depression, increased sensitivity to cold, and low blood pressure.
- Hyperthyroidism, on the other hand, is characterized by unexplained weight loss, anxiety, heat intolerance, and high blood pressure.
- There’s a higher incidence of thyroid disease in people with diabetes. While type 1 diabetes often coexists with autoimmune thyroid conditions, the relationship with type 2 diabetes is less direct but can be influenced by factors like weight gain.
- Regular thyroid testing is recommended for people with diabetes, especially those with type 1. Treatment options vary depending on the type of thyroid disorder, ranging from medication to more complex therapies like radioactive iodine treatment or surgery.
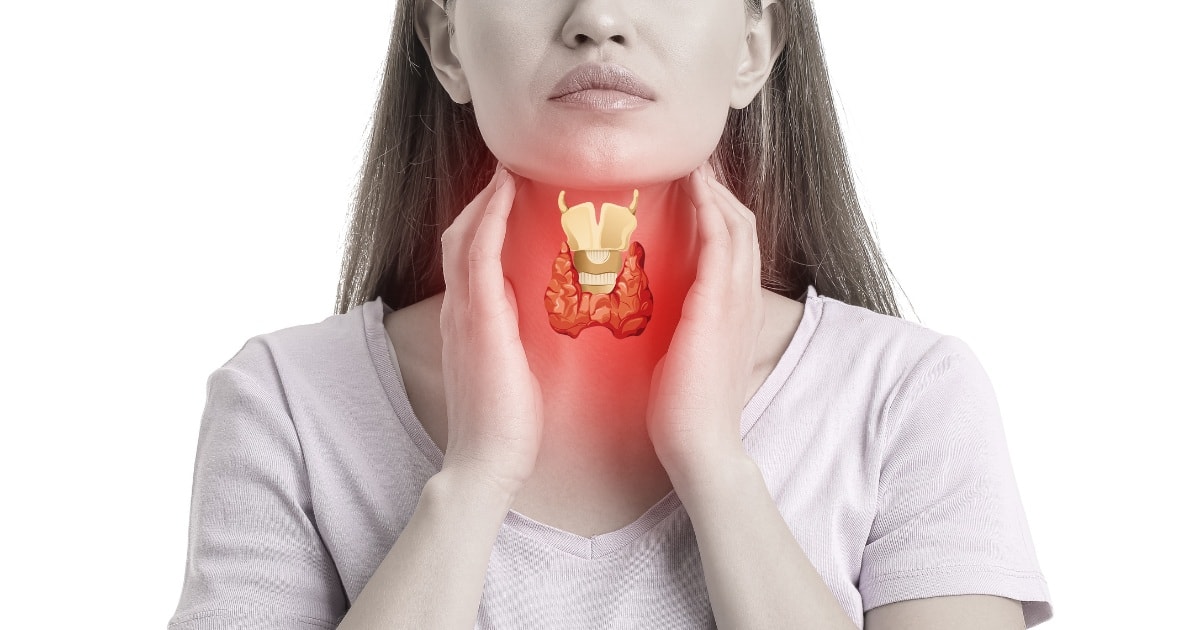
Your thyroid and what it does
Your thyroid is a hormone-producing gland that regulates the body’s metabolism. It’s located in the lower front of your neck.
This gland plays a critical role in regulating a number of things in your body, including your weight, energy, blood pressure, heart rate, mood, menstrual cycles, sex drive, and even your memory.
According to the American Thyroid Association (ATA), more than 12 percent of the U.S. population will develop a thyroid condition during their lifetime.
Although thyroid issues are common and easy to test for, the symptoms and test results can be easily overlooked or mistaken for other conditions. This can make an accurate diagnosis challenging.
Types of thyroid disorders
When the thyroid’s hormone production is impaired, you develop thyroid disease. The thyroid can either produce too little thyroid hormone (which is called hypothyroidism) or too much (which is called hyperthyroidism).
Causes of hyperthyroidism include Graves’ disease, thyroid nodules, and thyroiditis — inflammation of the thyroid. Hyperthyroidism is the less common of the two conditions, and only 0.5 percent of people living with type 1 diabetes will have hyperthyroidism.
Hypothyroidism is more common — both in the general population and in the diabetes population. Its most common cause is called Hashimoto’s disease.
It’s not clear why, but women are five to eight times more likely to develop thyroid issues than men.
Symptoms of hypothyroidism and hyperthyroidism
The thyroid gland plays a crucial role in regulating how the body uses energy, influencing the function of every organ.
Because of this, any imbalance in thyroid hormone production — either too much or too little — can lead to significant health effects. These imbalances impact the body’s metabolic rate and can affect everything from heart rate to body temperature.
The symptoms experienced due to these conditions can vary from person to person. You may experience some or all of the following symptoms:
- Unexplained weight gain
- Chronic fatigue
- Low blood pressure and slower pulse rate
- Depression
- Increased sensitivity to cold
- Constipation
- Tingling skin
- Irregular periods
- Low sexual libido
- Short-term memory loss
- Muscle cramping
- Hair loss and thinning
- Dry and rough skin
- Unexplained weight loss
- Chronic fatigue
- High blood pressure and increased pulse rate
- Anxiety
- Heat intolerance
- Diarrhea
- Itchy skin and hives
- Lighter periods
- Low sexual libido
- Difficulty with concentration
- Muscle weakness
- Hair loss and thinning
- Smooth, warm, or moist skin
How are diabetes and thyroid disease connected?
The prevalence of thyroid disease among people with type 2 diabetes is higher than in the general population, and 17 to 30 percent of people with type 1 diabetes have thyroid disease.
That’s a pretty stark contrast to the general U.S. population, where only 12 percent will develop a thyroid condition.
In other words, people living with diabetes are nearly twice as likely to develop thyroid disease compared to the general population.
However, that does not mean that diabetes causes thyroid disease, or vice-versa.
Are type 2 diabetes and thyroid disease connected?
As far as we know, there is no direct link between type 2 diabetes and thyroid disease.
The reason why many live with both thyroid disease and type 2 diabetes is because they are the most common endocrine diseases in the United States, according to R. Mack Harrell, MD, MBA, FACP, FACE, ECNU, Medical Imaging Director at the Memorial Center for Integrative Endocrine Surgery and Past-President of the American Association of Clinical Endocrinologists.
However, because factors like weight gain can contribute to the development of type 2 diabetes, there may be “indirect” links between thyroid disease and type 2 diabetes. If you gain weight due to hypothyroidism, that may put you at risk for type 2 diabetes.
Some studies have shown that people with prediabetes are 40 percent more likely to develop type 2 diabetes if they have untreated hypothyroidism.
Are type 1 diabetes and thyroid disease connected?
Much like type 1 diabetes, most types of thyroid disease are autoimmune disorders. Unfortunately, if you have one autoimmune disease, research shows that you’re more likely to develop others.
In type 1 diabetes, the immune system attacks the cells in the pancreas that make insulin. In some types of thyroid disease, the immune system attacks the cells of the thyroid.
Why people develop autoimmune diseases is not well understood, but there are many theories.
In an interview, Lowell Schmeltz, MD, FACE, Associate Professor, Oakland University William Beaumont School of Medicine Fellow, American College of Endocrinology, remarks: “There’s some genetic risk that links these autoimmune conditions, but we don’t know what environmental triggers make them activate.”
While research does not indicate that type 1 diabetes is actually causing thyroid disease, the diabetes diagnosis generally occurs first, with the thyroid condition developing at some point in the years afterward.
Can thyroid problems affect blood sugar levels?
Thyroid disease can have a major impact on your diabetes management and can increase a person’s risk of developing diabetes complications.
One of the ways that thyroid disease can sometimes be detected in people living with diabetes is if blood sugars suddenly (and consistently) become very erratic and hard to manage.
When your thyroid’s hormone production isn’t functioning normally, it will have a clear impact on your metabolism, which can indirectly affect blood sugar levels.
While the direct link between hypothyroidism and low blood sugar is not fully established, the condition can lead to changes in how your body metabolizes glucose. Hypothyroidism can slow down metabolism, potentially affecting how glucose is used and stored, which may affect blood sugar management.
Hypothyroidism is associated with changes in insulin sensitivity. In some cases, it can lead to decreased insulin sensitivity, where the body’s cells become less responsive to insulin.
This insulin resistance can make it harder for the body to lower blood sugar levels, potentially leading to high blood glucose. The slower metabolism associated with hypothyroidism also means that glucose may be processed more slowly, which can impact overall blood sugar management.
On the other hand, hyperthyroidism can increase the body’s metabolic rate, which might lead to a greater need for insulin due to the increased energy consumption.
This heightened demand for insulin can sometimes lead to difficulties in blood sugar management. In some cases, this can result in high blood sugar levels if the body cannot compensate for the increased need for insulin.
It appears that blood sugar levels can also affect thyroid function. The high blood sugar linked to hyperthyroidism can contribute to metabolic syndrome, a cluster of high blood sugar, high blood pressure, high triglycerides (blood fats), low HDL (“good”) cholesterol, and a large waist. Untreated, metabolic syndrome may develop into type 2 diabetes.
Research additionally suggests that the insulin resistance characteristic of type 2 diabetes may also be linked with the development of both hypothyroidism and hyperthyroidism.
When should you get tested for thyroid disease?
The American Diabetes Association Standards of Medical Care in Diabetes — 2024 recommends frequent screenings for thyroid disease in people living with type 1 diabetes.
People living with type 1 diabetes should be tested for autoimmune thyroid disease after diagnosis and have periodic follow-up screenings (every one to two years), even if they show no symptoms of thyroid disease.
There are no screening guidelines as such for people living with type 2 diabetes. However, some recommend that women over 50 living with type 2 diabetes should be tested regularly for thyroid disease.
How to test for thyroid disease
Often, all you need is a thyroid blood test (biomarkers: TSH, T3, and T4). It might also make sense for people living with type 1 diabetes to get a thyroid antibody test.
You can get tested for thyroid disease by visiting your doctor and asking for a blood test. Sometimes, a physical exam and a scan of the thyroid gland itself will also be recommended.
How to treat thyroid disease
If your test comes back out of normal range, you’ll need to discuss treatment options with your doctor. The good news is that thyroid disease is generally fairly straightforward to treat.
If you’re diagnosed with hypothyroidism, you’ll most likely be given a daily pill such as levothyroxine (brand names Synthroid, L Thyroxine, Unithroid, and others), which contains synthetic human thyroid hormone.
Your provider might have to adjust the dose a few times until your thyroid hormone levels are back in range. For most people, it’s a chronic condition, so you might need dose adjustment several times over the years.
If you’re experiencing uncomfortable symptoms, that may be a sign that your thyroid medication dosages need an adjustment with help from your medical team.
Treatment of hyperthyroidism is a little more complex and may include medication, radioactive iodine treatment (to decrease the overactive cells of the thyroid, preventing it from making high levels of hormone), surgery, or a combination of these. In some cases, hyperthyroidism resolves on its own.
In either case, making healthy lifestyle changes such as getting enough sleep, engaging in regular physical activity, eating balanced and nutritious meals, maintaining a healthy weight, and getting regular tests as recommended by your healthcare team can also help both your thyroid health and your general well-being.






Mike Gross
I’ve had hypothyroidism for 22 years, ciliac for 1.5 years, LADA for 1 year and have struggled with understanding and management of my issues. These articles are OUTSTANDING!!! What ways can I support the work you are doing?
Christel Oerum
We appreciate the comment. As long as you continue to read Diabetes Strong content, we’re happy
Tobias Oerum
Yes, thank you for catching that!