People with insulin-dependent diabetes take injections, lots of them.
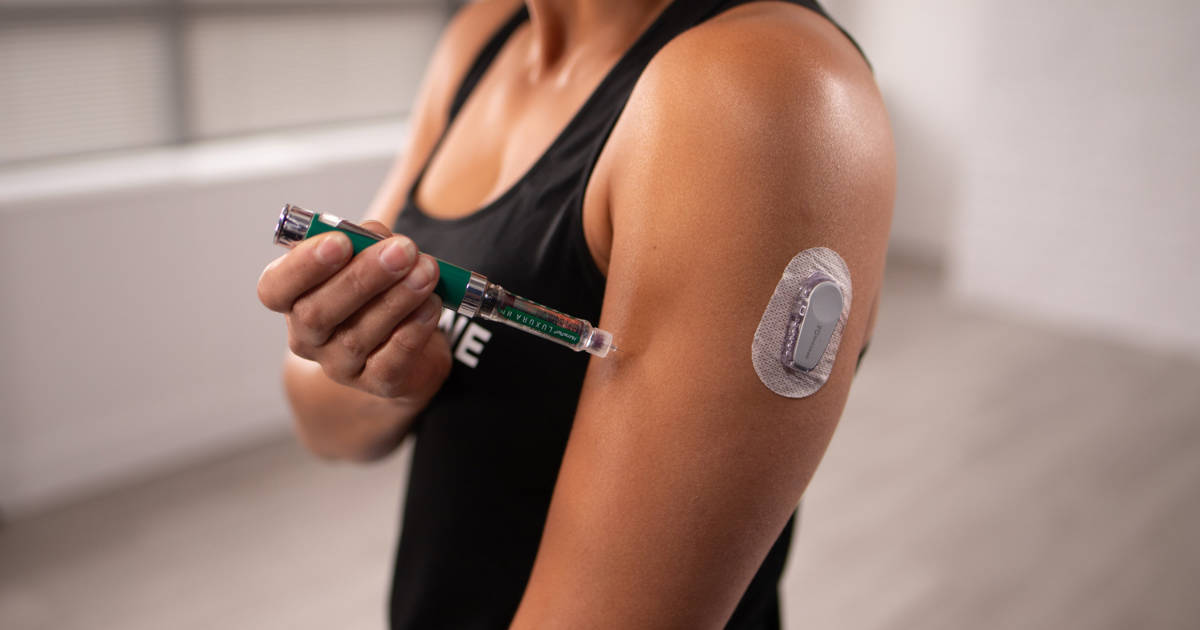
Management of insulin-dependent diabetes inescapably requires injections, whether, with multiple daily insulin shots, the use of a continuous glucose monitor (CGM), or even an insulin pump.
Injection site bruising, while not inevitable, can frequently occur. This article will outline strategies that you can employ to help avoid the nuisance, pain, and unsightliness of bruising at injection sites.
Why do people bruise at injection sites?
When you take an insulin injection, a bruise may typically appear because the small blood vessels under the skin are accidentally damaged, leaking their contents into the surrounding tissue.
It is perfectly normal to bruise from injections from time to time. Bruises from injections, while causing mild pain, are generally harmless and go away within a few days.
People with diabetes are more susceptible to bruising simply because we take so many injections. It’s bound to happen, but there are ways to reduce the incidence and severity of them.
Ways to reduce bruising
Try these strategies to help reduce the incidence of bruising when taking insulin injections.
You can start by watching this video where I show you how to inject and then read the detailed tips below.
Use longer needles
It may seem counterintuitive, but using shorter needles increases the likelihood that you will bruise.
When available, opt for longer syringe needles that will bypass the surface blood vessels, thus reducing bruising.
Inject at a 90-degree angle
While it may be easier to inject at a slant, try and inject at a 90-degree angle instead. This will improve the ease at which the needle goes into the skin, reducing the incidence of bruising.
Change your syringes and lancets more often
Most syringes and lancets are meant to be single-use, which can be a hard regimen to remember and stick to.
Changing out old lancets and only using syringes one time will ensure that the point at the tip of the syringe stays sharp and is significantly less likely to bruise the user.
Rotate sites!
Remember to rotate your injection sites. Routinely using the same sites (and even general areas) for your insulin injections will definitely cause bruising, and can even hasten the development of scar tissue, which can lead to malabsorption of insulin, leading to higher blood sugars.
Continuously rotating your sites can prevent all of this, including bruising!
Ice the area
Ice the site where you will be giving an injection about 30 to 60 seconds before doing so. Ice helps to shrink the capillary blood vessels under your skin, reducing the likelihood of damage and bruising.
Opt for technology
Although insulin pumps and continuous glucose monitor (CGM) technology are more expensive, opting for this type of diabetes management drastically helps to reduce the incidence of bruising, because site changes are far less often than multiple daily injections (MDI).
Insulin pump sites are changed anywhere from every 3-6 days, and CGM sites are changed anywhere from every 7-10 days, helping people with diabetes avoid the stresses of injecting or lancing themselves every day, multiple times a day.
Work with your doctor and insurance company to see if this can be a realistic option for you and your lifestyle.
Avoid your belly button
People love injecting insulin in their stomachs – there’s lots of space and usually a good amount of fat, which is excellent for insulin absorption.
However, injecting too close to your belly button will cause bruising and pain. Aim to avoid any insulin injections within an inch or two of your belly button.
Up your iron intake
People who suffer from anemia or low iron bruise much more easily. Your body needs iron to keep your blood cells oxygenated and healthy.
Without sufficient iron from sources like beans, lentils, tofu, dark leafy greens, or even a supplement, you will be more susceptible to bruising.
Aim for 8.7mg a day for men and 14.8mg a day for women, or check with your doctor if you think you may be suffering from anemia.
Calibrate your medications
Being on certain blood thinners, such as Warfarin, Plavix, or even over-the-counter aspirin may put you at a higher risk for bruising.
Work with your doctor and medical team to see if you can take alternatives if you’re struggling with bruising.
What to do if you develop a bruise after an injection
If you develop a bruise after an injection, fear not. Employ these helpful strategies to bring you quick relief:
- If you feel pain immediately after injecting, apply gentle pressure on the site to help prevent the development of a bruise
- Do not massage or rub the injection site, as this will make the bruise worse
- Treat the affected area with ice
- Do not inject insulin on or near the site until the bruise has healed completely
- If the pain is significant, treat it with ibuprofen to reduce inflammation
- If you’re struggling with chronic bruising, contact your doctor and medical team
Taking daily insulin injections can be painful, but it doesn’t have to leave lasting bruises on your skin.
Employing these strategies can help you drastically reduce the incidence of bruising when you inject insulin to manage your diabetes.



Rudy Dansak
Sometimes when inject insulin around my belly button I get a sharp tingle on the top of my hand, as if the nerves were directly connected.
It’s more of a curiosity than a concern.
Donna Zasgoat
I’m a rehab facility and have 1 nurses that always leaves me with thumbprint bruises. Granted I have a low on platelet count but should be bruised from this nurse all the time? She’s also hit a nerve once-had me seeing stars.
Christel Oerum
Hitting a nerve can happen to the best of us. But you’re absolutely right in your description it’s like seeing stars.
I would ask your doctor if he thinks the amount of bruising your experience is typical. And if you know you bruise less in certain places, you could ask the nurse to try one of those places
Randy Little
Needle lengths are not rated in ml. Ml is a volume. Needles are rated in gauge and LENGTH. What were you trying to say?
Tobias Oerum
You are absolutely right. We have removed that part and will update the article with more info soon.
Paul
Newly diagnosed diabetic. Thanks for the good read. Very helpful and even comforting.
melonie christian
i have bruising on my tummy and really paining what must i do
Christel Oerum
If you’re bruising abnormally and not healing, you should see a doctor. If it’s regular bruises, and there are no other underlying issues, they will heal with time.