If you live with diabetes, you probably know that it’s important to achieve good hemoglobin A1c (or HbA1c for short) levels.
But what exactly is an HbA1c? What is a “normal” HbA1c level, and how can you achieve and maintain that?
This article will dive deep into the numbers and explain the ever-elusive HbA1c.

What is an HbA1c test?
An HbA1c is a blood test that tells you your average blood glucose levels over the previous 2-3 months. HbA1c is short for “glycated hemoglobin test” or glycohemoglobin.
Hemoglobin is a protein found in your red blood cells, giving blood its red color, and its job is to carry oxygen throughout your body.
The HbA1c test, in particular, measures the average amount of blood glucose that has attached to the hemoglobin in your red blood cells over the past few months.
Red blood cells only live for about 3 months before regenerating. This is why the test will only show your average blood glucose for the previous 2-3 months.
How often should you test your HbA1c?
It’s recommended that people with diabetes get the test between 2-4 times per year (maybe more often, if the patient is pregnant or changing insulin therapy).
However, it is important to note that the test has some recency bias, and if your blood sugars have been higher for the previous several weeks before getting the test, your HbA1c number will also be higher.
It’s also important to note that the HbA1c test is an average of all your blood sugars from the previous few months, averaging all the highs and all the lows. This can sometimes give you a warped sense of what your blood sugar control actually is.
How does an HbA1c test work?
HbA1c tests are typically done in the lab and can either be done via a traditional blood draw (in the vein) or with a finger stick (with instant results).
If you have your blood taken via a blood draw from the vein, the results may take a few days to come back.
The test takes less than 5 minutes to complete, and unlike a fasting glucose test, you do not need to fast before taking the test, and it can be done any time of day.
You can also use an easy and reliable home testing kit to perform the test yourself.
In this video, Christel Oerum shows how easy it is to measure your A1c at home:
What is a “normal” HbA1c?
This depends on the person, but broadly speaking, HbA1c results are given in percentages:
- Normal, non-diabetic: HbA1c below 5.7%
- Prediabetes: HbA1c between 5.7% and 6.4%
- Diabetes (doesn’t decipher the type): HbA1c of 6.5% or higher
However, if you have gestational diabetes or existing diabetes, you will need to work with your doctor to figure out your individual health goals given your lifestyle, stage of life, and what will be sustainable for you long term.
Women who have existing diabetes and then become pregnant have stricter HbA1c goals for the duration of a pregnancy, for example. This number should usually be at or below 6%.
Seniors, and people who cannot easily feel their low blood sugars (also called “hypo-unaware”) may need to have a higher HbA1c goal, to prevent dangerous hypoglycemia (low blood sugar).
Athletes may also opt for higher HbA1c levels to make training easier and to maintain stamina, whereas newly diagnosed people with diabetes, still experiencing the “honeymoon phase” of intermittent insulin production from their pancreas, may have an easier time, and can aim for an HbA1c in the low to mid 5s.
However, if you do not have any lifestyle-specific goals and live with diabetes (any type), the American Diabetes Association recommends that you keep your HbA1c levels below 7% to below unnecessary complications.
Talk with your doctor to make sure you’re establishing individualized goals that will work for you and your life. There is no single “normal” HbA1c percentage that everyone should aspire to.
Related: How to Translate Your A1c to a Blood Sugar Level
Why is the HbA1c test important?
The HbA1c is most important for diagnosing diabetes, prediabetes, and even sometimes gestational diabetes (although a glucose tolerance test would be more efficient and beneficial in that case).
The Centers for Disease Control and Prevention (CDC) recommends that adults over the age of 45 get an HbA1c test to screen for prediabetes and diabetes. If the result is normal, your provider will recommend a schedule for re-testing based on your age and risk factors.
If your results show prediabetes, you should get a repeat test every 1-2 years. If you have prediabetes, you should talk with your doctor about steps you can take to reduce your risk of developing diabetes.
If you are under 45 years old, but exhibit certain risk factors, your doctor may also recommend an HbA1c test, including:
- Being overweight or obese
- Having hypertension (high blood pressure)
- Having heart disease
- Sedentary lifestyle/physical inactivity
No matter your age, you should call your doctor right away if you experience the following symptoms, as they are signs of diabetes:
- Extreme thirst
- Weight loss
- Blurry vision
- Extreme hunger, despite weight loss
- Fruity-smelling breath
- Extreme fatigue
- Body ache
- Headache
- Confusion
Your doctor may recommend you get an HbA1c test or seek emergency medical care, depending on the severity of your symptoms.
In people with existing diabetes, an HbA1c test is used to determine general diabetes control over the past few months.
It can potentially pick up issues you may be experiencing with both low and high blood sugar levels, and act as a guide to improving your health and preventing diabetes complications such as heart disease, retinopathy, kidney disease, high blood pressure, amputations, blindness, and premature death.
Studies have shown that even a 1% decrease in HbA1c decreases the likelihood of developing retinopathy by 37%!
Drawbacks of the HbA1c test
The standard HbA1c test has come under some scrutiny recently, simply due to the fact that it is just an average of high and low blood sugar levels.
With more and more people with diabetes adopting continuous glucose monitoring (CGM) technology, wider adoption of the Time in Range (TiR) measure of blood sugar control is gaining steam for people with existing diabetes.
Time in Range measures the percentage of your day where your blood sugar levels fall within a certain range (usually between 70mg/dL-180 mg/dL).
In this case, the higher the percentage, the better, because that means your blood sugar is experiencing fewer swings and is within a target range for the majority of the day.
Researchers think this is actually a better measure of overall control because you can pinpoint exactly where and when your blood sugar is spiking or dropping, and can see how much of your day your blood sugars are in a healthy range.
Because the HbA1c is just an average, it cannot give you the same detailed data and can sometimes be misleading. If you have many days with a high blood sugar of 400 mg/dL and lots of nighttime lows at 60 mg/dL, your HbA1c may still mistakenly give you a “healthy” percentage.
The graph below shows how three people can have the same average blood sugar but very different Time in Ranges.
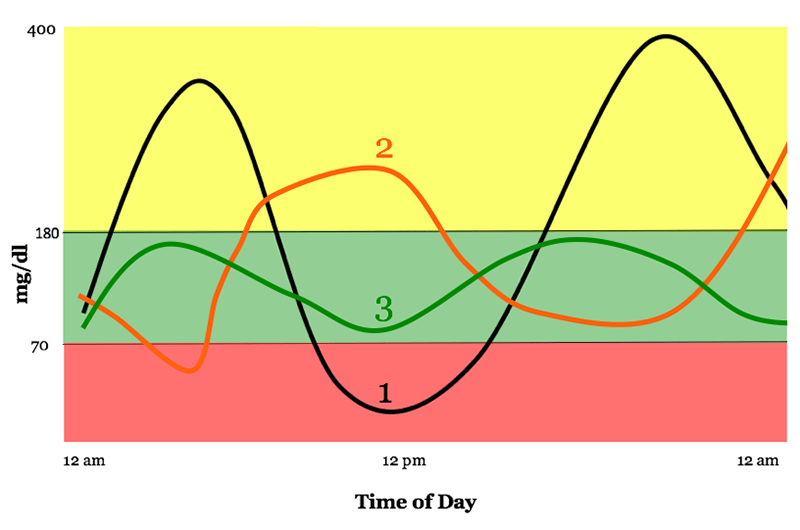
For the time being, most providers are relying on both the TiR and the HbA1c to give the best picture possible of their patient’s overall blood sugar management and control.
And, of course, for people without access to CGM technology, Time in Range isn’t possible, and they must still rely on the traditional HbA1c test.
To learn more about HbA1c and how to manage it, read our comprehensive guide: How to Lower Your A1c.




Rick
Thanks for this article. It’s a good reminder for me that A1c is just an average, and although it’s helpful, pairing the data with Time In Range provides a much clearer picture of your overall control.
Loraine
This is helpful, because I thought that my husband’s A1C at 6.7 was still too high, but I was comparing it with my own at 5.8 (which I know is also too high). So really, he’s doing good for having diabetes. Yeah! I think he does have range problems, though.
Sydney
I agree 100% with your statement:
_With more and more people with diabetes adopting continuous glucose monitoring (CGM) technology, wider adoption of the Time in Range (TiR) measure of blood sugar control is gaining steam for people with existing diabetes.
Time in Range measures the percentage of your day where your blood sugar levels fall within a certain range (usually between 70mg/dL-180 mg/dL). –
A1c is a tool in the toolbox but has drawbacks but the time in range is the ultimate and the shiniest tool in the toolbox so a CGM will become much more of a weapon against diabetes than a BGM or an A1c test.
I continue to believe in the Eversense E3 180 day CGM as the best on the market but you can’t go wrong with Dexcom or Libre either.