Does your blood sugar seem unpredictable at times? If you live with insulin-dependent diabetes, it most likely does, and sometimes it can be hard to determine what’s going on.
That’s why it’s important to learn how to calculate your insulin on board (IOB) because if you’re not paying attention to your IOB, your blood sugars will continue to seem random and unpredictable
While paying attention to your IOB will not solve all of your daily blood sugar woes, it can help you out immensely. It’s a key component to better diabetes management and something that is not brought up often or taught enough when you are diagnosed.
Knowing your IOB can help you successfully determine things like if it’s safe to go for a walk without your blood sugar going low, or if you should inject more insulin to correct a high blood sugar, or if you should eat a snack before bed so you won’t have to wake up in the middle of the night to treat a low blood sugar.

What is Insulin On Board
Insulin on board is how much active rapid-acting insulin you have in your body. I’ve also seen it described as BOB (Bolus On Board), or unused insulin.
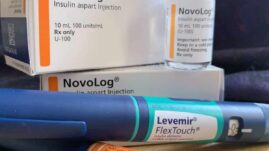
Rapid-acting insulin is the type of insulin people living with insulin-dependent diabetes use when we eat or need to correct highs. Common brand names of active insulin are: Humalog, Novolog, and Fiasp. It’s also the type of insulin that is used in insulin pumps.
Too much IOB will lead to low blood sugar (hypoglycemia) and too little to high blood sugars (hyperglycemia).
IOB is important since injected rapid-acting insulin can last in the body for 3-5 hours. That means that you should be paying attention not just to how many units of insulin you inject but also to how much is left of that dose up to 5 hours after your injection(s).
How long insulin is active in the body is a range (3-5 hours) because we all metabolize insulin at a slightly different rate. Most insulin pumps will be set to 3 hours, and most doctors recommend testing one’s blood sugar about 2 hours after a meal bolus, in part to check IOB and if a sufficient meal bolus was administered.
If you use an insulin pump, the pump will tell you your IOB from all boluses.
However, it’s worth noting that it does not include the basal (background insulin) which is also rapid-acting insulin. Overlooking the pump basal insulin when discussing active insulin is problematic especially for exercise, since too much IOB, from boluses or pump basal, will make blood sugars drop.
If you use insulin pens, there are a few apps available to help you calculate and keep track of your IOB such as RapidCalc (not FDA approved) or MySugr (EU only). There is also a smartpen called InPen available in the U.S.
How to calculate IOB
If you don’t have access to any devices or apps that calculate your IOB for you, or if you want to know your “pump basal IOB”, you can calculate your IOB fairly easily on your own.
In this video, I’ll walk you through examples of how to calculate your “pump basal IOB” and your IOB from injections.
I’d recommend going through the exercise of calculating your IOB a few times and start paying attention to how different levels of IOB impact your blood sugar in different situations.
Here are two additional examples
Basal IOB (pump) Example
Basal per hour is 1 IU, assuming insulin is active for 4 hours in the body:
1 IU x 25% + 1 IU x 50% + 1 IU x 75% + 1 IU x 100% = Total: 2.5 IOB
Bolus IOB (MDI) Example
1 IU injected 1 hour ago and 2 IU injected 3 hours ago, assuming insulin is active for 4 hours in the body:
2 IU x 25% + 1 IU x 75% = 1.25 IOB
Why you should care about IOB
Knowing your IOB can be a critical component to understanding if you have an adequate amount of insulin on board for a given activity. It’s the single best indicator of how your blood sugar will react during different times and activities.
One of the first things many people are taught after being diagnosed with diabetes is that stacking insulin is bad. Stacking insulin means taking more than one dose of rapid-acting insulin within the 3-5 hour timeframe while it’s active in the body.
But what if you didn’t get enough insulin during the first dose, should you just wait 3-5 hours while your blood sugars are high before correcting? Your IOB can help determine that.
When you calculate your insulin dose the IOB should be a component of the calculation. The calculation is this:
Insulin for the carbs you eat +/- Correction for your current blood sugar – IOB = Dose recommendation
So let’s say I’m not eating, my blood sugar is 250 mg/dL, my target blood sugar is 100 mg/dL, my correction factor is 50, and my IOB is 1 IU, this would be the calculation:
0 IU for carbs + 3 IU Correction dose ((250-100)/50)) – 1 IOB = 2 IU
Had I not taken IOB into consideration, I’d just have injected the 3 IU and most likely had gone low.
Another critical factor is reducing the risk of low blood sugars. The only reason why we go low is if we have too much insulin in our systems, too much IOB. So paying attention to our IOB needs for different activities is key to knowing if it’s appropriate for what we’re about to do or if we need a small carbohydrate snack first.
When is it important to pay attention to IOB?
While it is important to focus on IOB throughout the day, these are three of the most important times to pay special attention to it:
When you exercise
Your insulin sensitivity is heightened during and after exercise, increasing the risk of low blood sugar. By paying attention to your IOB, and how your blood sugars react when you do different types of exercise, you’ll be able to adjust your IOB (by adjusting your insulin in the hours before you exercise) so that you can exercise with balanced blood sugars.
And in those situations where you can’t plan ahead, you’ll know if you have too much IOB and you’ll need a carbohydrate snack.
Before bed
Getting a good night’s sleep can be hard with diabetes and no one wants to deal with low blood sugars at night or waking up with a blood sugar hangover after having high blood sugars all night.
Checking your IOB and blood sugars before bed can help you assess if it’s safe to go to bed, if you need a snack to prevent a low blood sugar, or if you should take a correction dose for a high blood sugar.
Before meals or corrections
IOB should be part of every meal and correction calculation and can make your insulin doses more precise.
Knowing your IOB allows you to dose when needed, eat when you feel like it, and it helps to build confidence in the insulin doses you take.


Sjw productions
The description of calculating IOB is incorrect here at a basic level. IOB is any active insulin dosed greater or less than your basal insulin dose throughout the day and night. Therefore, with a AID pump does not match your description. Any insulin pump that uses variations in basal can deliver less than or more than the programmed basal insulin. This means that IOB can become a negative or positive amount added to the programmed basal dose amount. And as you describe, the duration of the insulin action time also plays a roll in calculating the IOB.
Loni Devlin
I fast 18 hrs and a lot of times when I wake up my blood sugar is over 200?? Why does it go up. Also I will go to PT and work out on that same fast and it will go up?? How come??
Christel Oerum, MS
I explain why that happens and what you can do to try and prevent it in this video: https://youtu.be/-O5aRAnn9T0?si=iu6SDPs5oEbZ8Lk-