If you’ve recently made the change to insulin pump therapy from multiple daily injections (MDI), the change in treatment may be overwhelming and confusing.
You’ll need to change many aspects of your day-to-day life, including what type of insulin you may take.
Not all types of insulin will work in insulin pumps, so you need to be careful when making the change. This article will investigate which types of insulin are appropriate for insulin pump therapy, and which are not.
Always advise your doctor before making any changes to your treatment, especially when you’re switching from MDI to insulin pump therapy.
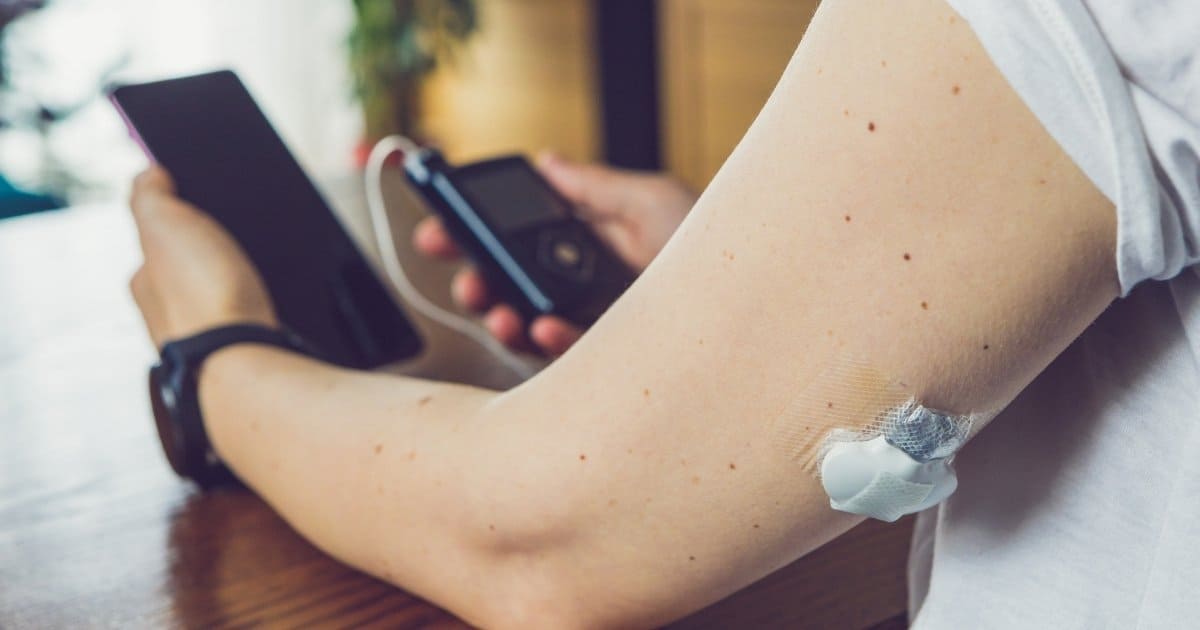
How does insulin pump therapy work?
Instead of manually taking insulin injections for everything one eats (plus one or two “long-acting” insulin injections daily), insulin pump therapy works by giving a small amount of fast-acting insulin continuously underneath the skin with an infusion set that the patient operates remotely, either from a personal diabetes manager (PDM) or insulin pump.
Since the drip of insulin acts as a basal insulin, it is normally a fast-acting insulin that one uses both for basal and bolus administration of insulin.
Can any type of insulin work in an insulin pump?
No. It’s crucial that you work with your doctor to determine which insulin will work best for you in your insulin pump, but strictly speaking, only fast-acting insulins, such as Aspart (Novolog and Fiasp), Lispro (Humalog and Lyumjev), and Glulisine (Apidra) can safely be used in insulin pumps.
The two newest (and fastest) insulins are Fiasp and Lyumjev which anecdotally take effect within 5 minutes of administering them. They have both been approved for use in insulin pumps and are an excellent choice if you struggle with pre-bolusing for meals (they can even be taken after eating a meal, especially if you’re eating low/slow carb.)
Note: Fiasp is currently not recommended for the Tandem T-Slim pump as Tandem has not conducted studies to verify its safety and efficacy in its system.
Regular insulin, such as Humulin and Novolin R, while not as commonly used anymore (except in some medical situations and sometimes in people with type 1 diabetes and type 2 diabetes who maintain a strict Ketogenic diet), may be used in insulin pumps, but it is not always recommended.
Fast-acting insulins are better for insulin pumps due to the mechanism by which the insulin in an insulin pump is dispensed continuously.
This continuous basal rate replaces the need for long-acting insulin shots, like Glargine (Lantus, Basaglar, and Toujeo), Detemir (Levemir), or Degludec (Tresiba).
Since long-acting insulin’s effectiveness is delayed on purpose, this would create a disaster if administered in an insulin pump, without the patient getting immediate insulin, and causing serious blood sugar crashes later on in the day.
The type of insulin you can use in your insulin pump will be further determined by your insurance coverage, what your doctor prescribes you, and your preferences.
You can learn more about the different types of insulin in our guide “Insulin Types: Their Peak Times and Durations”.
Why only use fast-acting insulin?
In short, fast-acting insulin will achieve better blood sugar levels and result in better control for the patient than using longer-acting insulin in pumps.
The benefit of fast-acting insulin is that they take effect immediately: usually within 10-15 minutes of administration, and they peak after about an hour.
The total duration of fast-acting insulin in the body is between 3-4 hours, depending on your metabolism and ability to process the insulin.
Additionally, using fast-acting insulin in an insulin pump can better manage high blood sugar levels, whereas trying to manage your blood sugars with long-acting insulin alone is cumbersome and dangerous, due to their delayed effects, multiple peaks, and long duration in the body.
Can I get rid of long-acting insulin forever?
In theory, yes, but it is always helpful to have a prescription for long-acting insulin on hand (and preferably, a few spare vials of long-acting insulin in your refrigerator!).
Insulin pumps, like all technology, can break down from time to time, and it’s helpful to have a backup mechanism for taking insulin and managing your diabetes if something goes wrong.
Sometimes when an insulin pump breaks, it can take a few days to have the manufacturer ship a new one out to you, and you don’t want to be waking up every two hours throughout the night just to take a mini bolus of fast-acting insulin (in place of a long-acting shot once or twice per day!).
Ask your doctor for a spare prescription for Glargine (Lantus, Basaglar, and Toujeo), Detemir (Levemir), or Degludec (Tresiba), so if you have to, you can resort to multiple daily injections (MDI) without too much of an interruption to your diabetes management.
You may also wish to go on an insulin pump “break” from time-to-time as well. People who are very active in the summertime, play a lot of water sports, or want to swim in a pool or ocean without worrying about an infusion site may wish to take a break from the patches and tubing and go back to manual injections as well.
Having some spare long-acting insulin nearby can be helpful for that, or even if you’re just feeling burnt out on insulin pump therapy in general.
For more about the potential problems with taking insulin, read “Insulin Side Effects: What You Need to Know”.
Are there any downsides to using only fast-acting insulin?
While there are not too many downsides to using only fast-acting insulin in an insulin pump, it does increase your risk of developing high blood sugars and even diabetic ketoacidosis (DKA) should something go wrong with your insulin pump, including a bent cannula, pump malfunction, or damaged insulin pump.
This is because of the mechanism of fast-acting insulin, and the fact that it’s usually completely out of one’s system within 3-4 hours of administration.
If one’s insulin pump malfunctions overnight, a person with diabetes may be without any active insulin in their body for hours on end, which can be dangerous.
People who are on MDI and take both fast- and long-acting insulin always have that backstop of long-acting insulin in their system to prevent the onset of DKA (in most cases).
Additionally, if you forget to bolus for a meal, you may experience higher blood sugars as a result of not having that long-acting insulin in your body as that backstop as well.
There are pros and cons to being on an insulin pump with only fast-acting insulin versus being on multiple daily injections (MDI) with a mix of long- and fast-acting insulin, and it will be up to you (under the guidance of your doctor!) to make the best choice for you and your diabetes.
You can read the article “Why I Choose Multiple Daily Injections over an Insulin Pump” to learn more about the pros and cons of MDI and insulin pumps.
Conclusions
Insulin pumps are an incredible piece of diabetes technology that work by releasing a small amount of insulin regularly throughout the day, in a continuous drip, just like a natural pancreas does in someone without diabetes.
This small amount of insulin dispensed by the insulin pump is called a basal rate, and everyone differs.
You will need to work with your doctor to determine an appropriate basal rate and bolus structure for you, your diet, your goals, and your lifestyle.
One thing is constant, however. Only fast-acting insulin (and occasionally Regular insulin) is deemed appropriate for insulin pumps.
This is because the continuous drip of fast-acting insulin replaces the need for a long-acting insulin injection once per day. That same fast-acting insulin also acts as the bolus insulin, administered by the patient, on their insulin pump.
Fast-acting insulin, in an insulin pump, is used for both basal and bolusing purposes, with zero long-acting injections required.
This all may sound confusing at first, but it actually makes life easier for people with diabetes.
You can learn more about insulin therapy in these articles:




Bob Malin
While I have no desire to be on a pump, reading that a pump can in essence get rid of a long acting insulin leaves me confused. I had tried just fast acting insulin and I was fine. I feel like the long-acting I am taking, it just sits in my body and has lead to weight gain. If my dexcom goes off anyway cause of a high-blood in the middle of the night, why do I even need to bother with long-acting? I would really love someone to chime in. I am currently on 32u of basaglar and bolus for meals with humalog. Thanks, Bob
Glenda M Calcutta
FIASP is not recommended for all pumps…not allowed for Tandem T-slim
Tobias Oerum
You are correct and thank you for pointing that out. We have updated the article.