For people with insulin-dependent diabetes, the near-constant attention to detail can sometimes be taxing on our mental health.
While perfection is impossible, diabetes demands a lot of precise measuring, counting, and dosing of food, exercise, and especially insulin.
But we’re human. We are bound to forget to take a dose of insulin from time to time. This article will detail exactly what you should and shouldn’t do if you miss a dose of insulin.
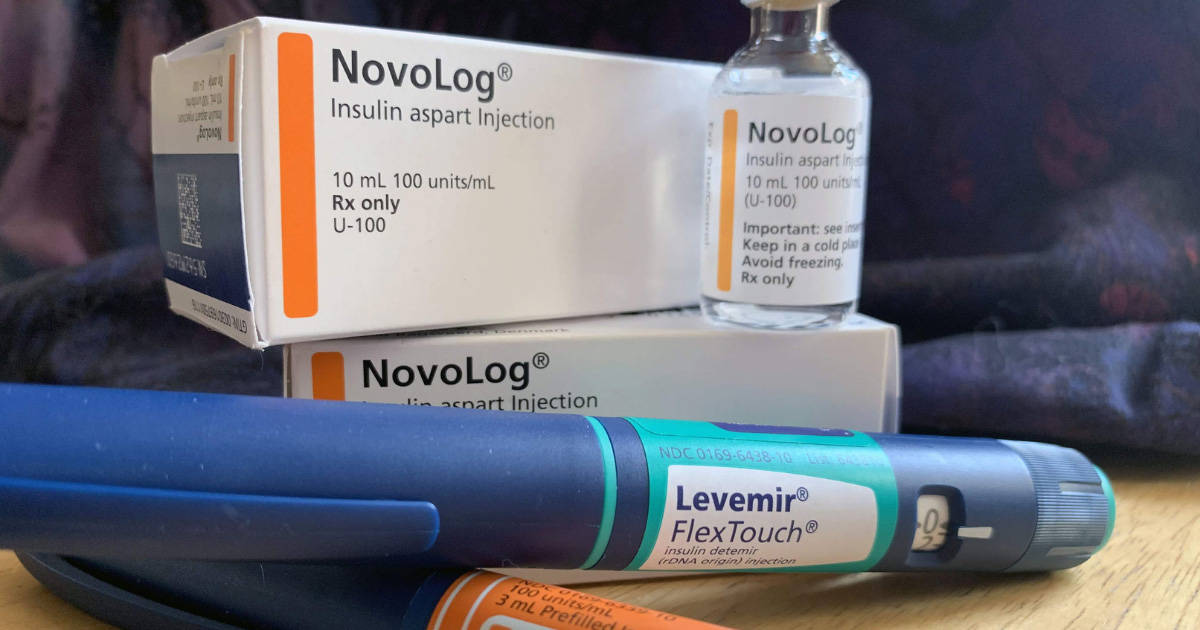
What would cause someone to forget to take insulin?
Literally anything can cause someone to forget to take their insulin: traveling, time-changes, sleepovers, the weather, falling asleep before a scheduled dose, an interruption such as a phone call or text message, spontaneous meals or snacks, or even just being forgetful are common reasons.
This is perfectly normal and happens to everyone. Do not guilt yourself or feel down if you forget to take your insulin from time to time. It may happen, but these strategies can help.
What to do if you miss a dose of insulin
Implement these strategies if you’ve missed a dose of insulin to get back to feeling better as soon as possible:
Make sure you’ve actually missed a dose
There’s nothing worse than being halfway through a dinner out with friends, thinking you’ve forgotten to bolus for your food, and taking twice as much insulin as you need as a result (dessert, anyone?).
It’s helpful to always announce, or at least tell one other person when you’re bolusing for a meal or taking nighttime long-acting insulin , as two minds are better than one at remembering! Sometimes insulin injections all blur together, so having an extra set of eyes and eyes on your dosing can help.
This risk is slightly lower if you’re on an insulin pump, as you can simply go into the settings and check your bolus history to see if you in fact have missed a dose.
Technology such as smartpens that send data to an accompanying app can also help you track both insulin on board and doses already given. You can watch this review of the InPen to learn more:
If you have indeed missed a dose, proceed, if not, definitely do not double dose!
Don’t panic
Missing a single dose of insulin will probably not kill you. The great thing about insulin and diabetes is that you’ll always need more, so if you forgot a dose, it’s not the worst thing in the world.
The bad thing is that you’re now chasing a high blood sugar, instead of preventing one in the first place.
Self-blame and feelings of guilt have no place here; diabetes is a marathon, not a sprint, and if anyone else is making you feel bad about missing a dose, politely ask them to walk a mile in your shoes.
Take insulin as soon as possible
As the heading suggests, it’s best to take your insulin as soon as possible, but there are some caveats.
If you simply forgot to pre-bolus for a meal, and you’re still within a 30-minute window of eating, you should count carbohydrates and bolus for the meal like you would regularly do.
If you’ve eaten more than a half-hour ago, it’s best to treat the high blood sugar you (most likely) have, instead of trying to count carbohydrates that are now being digested. This helps prevent unnecessary hypoglycemia if you take too much insulin.
If you’ve missed a dose of your long-acting insulin, it’s best to call your Endocrinologist right away to determine how much of the remaining dose you should take, based on how much time has passed since your typical time of administration, etc., unless it’s within a window of an hour or so of your normal dose.
If that’s the case, you can most likely proceed as normal (just be cognizant that now you’ll have active insulin for an hour longer, likely affecting the timing of tomorrow’s dose).
Test for ketones
Ketones are toxic chemicals that build up when your body starts to burn fat for energy instead of glucose. The most common cause of ketones for people with diabetes is lack of insulin.
Without insulin, glucose builds up in the bloodstream, because it cannot enter the cells. The result is ketones forming in the blood and eventually spilling out into the urine which can be picked up and measured by a ketone strip (found at pharmacies or on Amazon).
If your blood sugar is over 250 mg/dL and it’s been longer than a half-hour since you finished your meal, test for ketones. This will help inform the amount of insulin you’ll need to treat the high blood sugar.
If your ketones are moderate or high, call your Endocrinologist for guidance on how much extra insulin you’ll need on top of your normal correction factor (some people require up to 75% more insulin if they have high blood sugars and moderate ketones).
If your blood sugar and ketones will not come down and dissipate within a few hours, you will need to seek emergency medical care for fluids and an intravenous insulin drip.
Drink water
Water helps break up glucose in the body and prevents insulin resistance; this is especially important if you’re dealing with high blood sugar from a missed dose.
The U.S. National Academies of Sciences, Engineering, and Medicine recommends that appropriate daily fluid intake is about 3.7 liters per day for men and 2.7 liters per day for women (more if you exercise).
Drink up, especially after missing a dose of insulin.
Test every two hours
It is crucial to test every two hours after a missed dose (+ correction) to determine if you need more insulin and to stave off the dangers of diabetic ketoacidosis (DKA).
If you have a continuous glucose monitor (CGM) this will be easier, but it is super important to keep a close watch on your blood sugars for at least 12 hours after a missed dose.
This can be harder some times throughout the day than others: for instance, you may need to set an alarm to go off every two hours during the night, which isn’t pleasant but is necessary.
What not to do if you forget to dose insulin
While it’s important to be action-oriented, here are some things you should never do if you forget to dose insulin:
- Blame yourself
- Call the whole day a wash and let yourself have high blood sugars the rest of the day
- Go to sleep immediately
- Not take a correction dose of insulin at all
- Not tell anyone about the missed dose
- Bolus like normal for the number of carbohydrates you ate, even if you ate several hours before realizing you missed a dose
- Take double the amount of insulin for carbohydrates eaten and high blood sugar, without factoring in the time that has passed, carbohydrates already digested, or your blood sugar correction factor (or calling your doctor for help)
Ways to remember to take insulin
While no one is perfect, here are some tricks and tips to help you remember to take your insulin:
- Take your long-acting insulin at the same time every day
- Build it into your morning routine (first, brush your teeth, then wash your face, then take insulin)
- Set an alarm on your phone to remind you to take a long-acting dose or meal boluses
- Put a reminder up on a daily schedule to take your insulin
- Eat the same or similar foods every day, so bolusing for meals is easier
- Write down once you’ve given your insulin, so you don’t take it twice!
- Ask a partner or friend to remind you to take your insulin before all meals that are eaten together and let them know once you’ve done it
There is no place for perfection in a life with diabetes, and forgetting to take one’s insulin is bound to happen from time to time.
It’s best not to blame yourself, correct the mistake, and move on with your day. Tomorrow is a fresh start and a new beginning, and you will undoubtedly have ample opportunities to not forget to take your insulin again next time.


Robert Jette
I have been sick today and take Toujeo every morning. I forgot and now don’t want to take and then again in the morning doubling. I covered the high blood sugar with short acting and checking every 2 hours. Then will take my normal dose in the morning as usual. Is that correct?
Christel Oerum
Toujeo lasts beyond 24 hours in the body (up to 36 hours). So if you have forgotten it you won’t have any long-acting insulin in your body after ~24-36 hours. This you can cover with rapid-acting insulin as long as you give yourself a dose every 3-4 hours. You don’t want to be in a situation where you have no insulin on board (long or short) as that can lead to DKA.
Bonnie D
I am at work and left my novolog pen at home, will it hurt me to miss my lunch time injection?
Christel Oerum
Your blood sugar will go high, but if you still have an insulin production, or have long acting insulin onboard the risk of DKA is small. But I would rush home and take the dose as soon as you can
Juana Cruz
What to do if I missed a lantus long acting insulin? Do I waiting till the following morning? My blood sugar was low before dinner.
Christel Oerum
I think it depends on how much time goes by before you notice. It’s a good discussion to have with your doctor as it depends on whether you have any insulin production left. If you don’t he/she might suggest you take at least 1/2 your dose later in the day
Paula cook
I am not certain if I took it. I woke at four and ate cereal.
Bryan
Hey, my names Bryan. I’ve been a type 1 diabetic since I was 4 (29 now). I accidentally took my Humalog insulin instead of my tresiba insulin. I’m supposed to have 5 of humalog in the morning than 8 for supper than before I’m suppose to take 18 of tresiba. But tonight I mixed up my morning insulin with my night insulin. My question is l, what do I do when I wake up? Do I take my regular dosages? Do I not take anymore humalog the following day ?
Christel Oerum
Humalog only works in the body for 3-5 hours so you might have run a bit high overnight but by morning you should be able to get back into your usual dosing routine
Margaret June
Bryan, This EXACT situation occured within the first week of our son’s diagnosis. He was 8 years old at the time, his dad panicked while I called his endocrinologist. Easy enough they told us no harm done, this was extremely common. If he went low bring him back up just like any other low. Wait 24 hours without any insulin then back to normal schedule. Obviously call again with any further questions or concerns.
carol Anderson
I take 40 units of insulin before I go to bed at night. I just realized I am out of insulin. My sugars right now are 11.l (Canadian). I won’t be able to fill my prescription until the morning. Is it ok to just miss one shot?
Christel Oerum
If your body doesn’t make insulin you’ll be at high risk of going into DKA. I would test for ketones and consider going to the ER for an emergency insulin dose (depending on the ER they might give you an insulin pen)
Paula Seitz
did not have enough insulin, can’t get a refill, for a 75/25 pen