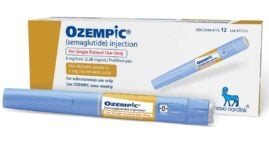
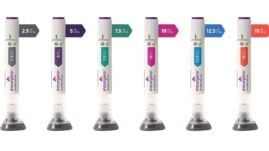
Ozempic and Mounjaro are both popular injectable medications used to treat blood sugar levels in adults with type 2 diabetes.
This guide will explain the key differences between Ozempic and Mounjaro and help you decide which medication you should choose.
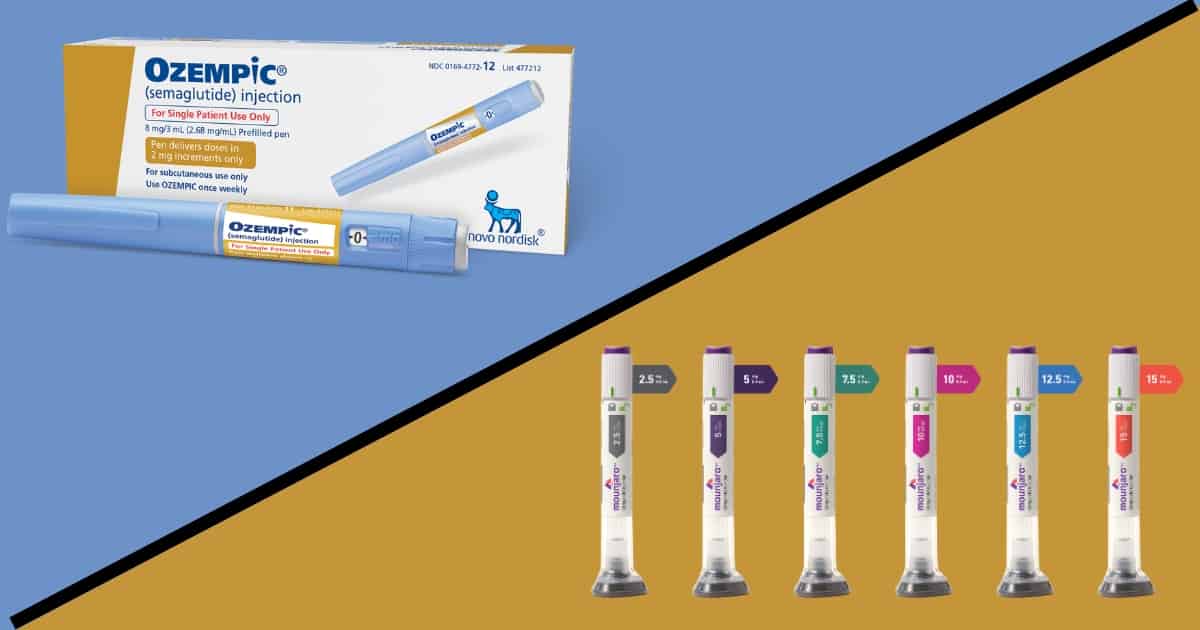
Key Points:
- Ozempic’s active ingredient is semaglutide, which mimics GLP-1 hormones.
- Mounjaro’s active ingredient is tirzepatide, which mimics both GLP-1 and GIP hormones.
- Both drugs lower blood sugar and A1c levels, improve insulin sensitivity, decrease insulin resistance, and may lead to weight loss.
- At the maximum doses, Ozempic has been shown to lower A1c from 1.4 to 2.1 percent, while Mounjaro averages a reduction of 2.3 percent.
- Both medications have shown potential in supporting cardiovascular health.
- It’s crucial to never mix or use Ozempic and Mounjaro simultaneously due to their different active ingredients and mechanisms.
Table of Contents
- What are the active ingredients in Ozempic versus Mounjaro?
- Why do people take Ozempic or Mounjaro?
- How are Ozempic and Mounjaro similar?
- How are Ozempic and Mounjaro different?
- Can I switch between the two drugs?
- Is Ozempic better than Mounjaro?
- How much do Ozempic and Mounjaro cost?
- Patient assistance programs
- Can I get off my other diabetes medications if I lose enough weight on Ozempic or Mounjaro?
What are the active ingredients in Ozempic versus Mounjaro?
Ozempic and Mounjaro are similar drugs, but they should not be combined or used at the same time. This is because they have different active ingredients and mechanisms of action.
Ozempic’s active ingredient, semaglutide, specifically mimics GLP-1 hormones in the body, which play a role in decreasing appetite, slowing stomach emptying, reducing the release of glucose from the liver, and increasing insulin release.
On the other hand, Mounjaro’s active ingredient, tirzepatide, has a dual function. It mimics both GLP-1 and GIP incretin hormones, hence its nickname “twincretin.”
While it shares GLP-1’s effects, the addition of GIP action enhances insulin release in response to high blood sugar and plays a role in fat metabolism.
The combined activity of GLP-1 and GIP in Mounjaro offers a broader approach to regulating blood sugar levels and appetite compared to GLP-1 alone.
Why do people take Ozempic or Mounjaro?
Ozempic and Mounjaro are both used in the treatment of type 2 diabetes.
They are liquid, injectable medications that help lower blood sugars and A1c levels and are taken subcutaneously (just under the skin) in areas such as the abdomen, thigh, or upper arm.
Both drugs help improve insulin sensitivity while decreasing insulin resistance.
Another notable effect is that they also slow digestion and suppress appetite. As a result, many people who take these medications experience weight loss.
Read more in: Can Ozempic Help You Lose Weight? and Can Mounjaro Help You Lose Weight?
Ozempic and Mounjaro also help lower the risk of heart attack and stroke in people with type 2 diabetes and heart disease.
People may be prescribed Ozempic or Mounjaro “off-label” — in a manner not officially approved by the U.S. Food and Drug Administration (FDA) — to improve insulin resistance and help with weight loss.
Neither Ozempic nor Mounjaro are FDA-approved specifically for weight loss. However, the FDA has approved a medication called Zepbound for this purpose.
Read more in: Everything You Need to Know About Zepbound.
Zepbound is chemically identical to Mounjaro, containing the same active ingredient at the same strength, but it is marketed under a different name when used for weight-loss treatment.
People are not prescribed both Ozempic and Mounjaro simultaneously. You may take one or the other. Never mix the two medications.
How are Ozempic and Mounjaro similar?
Ozempic and Mounjaro can be used alone or together with other diabetes medications.
The two medications are similar in the following ways:
Lower blood sugar and A1c levels
Both Ozempic and Mounjaro have been proven to lower blood sugar and A1c levels.
People who take the maximum dose of Mounjaro (15 milligrams [mg] per week) lower their A1c by an average of 2.3 percent.
People taking Ozempic can lower their A1c by 1.4 to 2.1 percent, on average.
As outlined earlier, these medications lower blood sugar through multiple mechanisms: they increase insulin secretion in response to high blood glucose levels, inhibit the liver from releasing excess glucose into the bloodstream, and improve overall insulin sensitivity.
Additionally, they indirectly contribute to better blood sugar management by slowing stomach emptying and reducing appetite.
May cause weight loss
Neither medication is FDA-approved as a weight loss drug. However, studies have shown that both drugs can help people lose weight.
Ozempic suppresses appetite and slows digestion, which aids in weight loss.
One study reports that over the course of 40 weeks, people taking 1 mg weekly of Ozempic lost an average of 13 pounds. Those taking 2 mg weekly lost an average of 15 pounds.
In other studies, Mounjaro helped people lose 12 to 15 pounds on a 5-mg weekly dose, between 15 and 21 pounds on a 10-mg weekly dose, and between 17 and 25 pounds on a 15-mg weekly dose.
There is no recommended dose to take for weight loss since these medications aren’t approved for weight loss by the FDA. (For Zepbound, the weight-loss version of Mounjaro, available doses are 2.5 mg, 5 mg, 10 mg, and 15 mg taken by injection once weekly, with 15 mg being the maximum dose.)
Learn more about administering these medicines in: Ozempic Injection: Where and How to Inject and Mounjaro Injection: Where and How to Inject.
Talk with your doctor if you’re interested in losing weight. They can provide you with information on both pharmaceutical and lifestyle approaches that can help.
Lower cardiovascular risks
These medications support cardiovascular health, which is important for people living with diabetes.
In studies, after 52 weeks, participants on the highest dose of Mounjaro (15 mg per week):
- Lowered their total cholesterol by about 5.6 percent
- Lowered their triglycerides by 22.5 percent
- Lowered their LDL (“bad”) cholesterol by 7.9 percent
- Lowered their VLDL cholesterol by 21.8 percent
- Increased their HDL (“good”) cholesterol by 10.8 percent
Additionally, a meta-analysis (analysis of data from several clinical trials) from The Lancet found that Ozempic lowered cardiovascular risk and even decreased the risk of death in people with diabetes and heart disease.
The American Diabetes Association (ADA) recommends GLP-1 agonists for people who have type 2 diabetes and heart disease to lower cardiovascular risk.
In addition to taking Ozempic or Mounjaro, a healthy diet and an increased amount of physical activity can go a long way to improving your heart health.
May cause adverse side effects
Both Ozempic and Mounjaro can cause mild to severe side effects, especially when you first start taking the medication.
Side effects of these medications include:
- Nausea
- Vomiting
- Diarrhea
- Constipation
- Low blood sugar, especially when used in conjunction with insulin
They also may cause serious side effects, including:
- Pancreatitis
- Kidney problems
- Increased risk of thyroid cancer
- Allergic reaction
Learn more in: Ozempic Side Effects: What You Need to Know and Mounjaro Side Effects: What You Need to Know.
They do not replace insulin
Ozempic and Mounjaro do not replace insulin.
If you decide to begin treatment with one of these medications, you will still need to continue taking your other diabetes medications as prescribed.
Your insulin needs may go down over time as a result of improved insulin sensitivity, but you’ll most likely not stop insulin treatment altogether.
They can be taken with or without food
Unlike insulin, these medications do not cause acute low blood sugar levels and they can be taken with or without food.
Eat something bland like toast, a banana, or crackers to alleviate any nausea you may experience after your injection.
They may worsen diabetic retinopathy
These medications may cause or worsen diabetic retinopathy, especially when you first start taking them.
Studies show that semaglutide, the active ingredient in Ozempic, is associated with the early worsening of diabetic retinopathy.
Similarly, tirzepatide, the active ingredient in Mounjaro can make diabetic retinopathy worse.
Although this side effect does not occur in all people who take these medications, the drugs do come with an increased risk of vision changes and worsening vision.
Talk with your doctor if you have early-stage diabetic retinopathy or are concerned that taking Ozempic or Mounjaro may impact your eye health.
How are Ozempic and Mounjaro different?
It is important to note the key differences between these medications so you can make the healthiest and best choice for you.
The two medications are different in the following ways:
The dosing will differ
Ozempic and Mounjaro have completely different dosing schemes, and they are not interchangeable.
The doses for Ozempic are the following:
- New to treatment: 0.25 mg once per week for the first four weeks.
- Ongoing treatment: 0.5 mg once per week starting on week five. If your doctor thinks you require more, there are doses available in 1-mg and 2-mg pens.
Read more: Ozempic Dosage Guide: How Much Should You Take?
The doses for Mounjaro are the following:
- New to treatment: 2.5 mg once per week for the first four weeks.
- Ongoing treatment: 5 mg once per week starting on week five. If your doctor thinks you require more, there are doses available in 7.5-mg, 10-mg, 12.5-mg, and 15-mg pens.
Read more: Mounjaro Dosing Guide: How Much Should You Take?
Since the active ingredients are different, these doses are not interchangeable and it can be very dangerous if you attempt to use them in this manner.
They have different active ingredients
The active ingredient in Ozempic is semaglutide and the active ingredient in Mounjaro is tirzepatide.
Tell your doctor if you are allergic to one or the other’s active ingredients so that they can prescribe you an alternative.
Can I switch between the two drugs?
This may be possible, as long as you do not have any allergies to the ingredients of the other medication.
If you’re experiencing severe adverse side effects on one drug, you may wish to try another to see if your body will adjust better to it.
However, if you’ve been taking Ozempic, you will need to wait a full week from your last dose before beginning your first dose of Mounjaro.
Only switch medications under the guidance of your doctor. The dosing is completely different between the two medications and it does not translate between them.
Even if you’re on the highest dose of Ozempic, your doctor will probably start you on a small dose of Mounjaro (and vice versa) until your body gets used to the new active ingredient.
Is Ozempic better than Mounjaro?
Individual responses to these medicines vary, and what is better for one person may not be better for another.
In studies, Mounjaro has been shown to lead to improved blood sugar management and greater weight reduction than Ozempic. However, Mounjaro is more expensive and may cause additional side effects. Ozempic is also FDA-approved to reduce cardiovascular risk.
How much do Ozempic and Mounjaro cost?
The out-of-pocket cost for Ozempic and Mounjaro depends on your insurance plan, including any co-pays or deductibles that apply to you. Both medications are commonly covered by insurance for the treatment of type 2 diabetes, but coverage may vary when prescribed for off-label purposes, such as weight loss.
To check your exact co-pay or coverage for either medication, you can use your prescription or medical insurance card to access the manufacturers’ co-pay calculators:
Ozempic Co-Pay and Coverage Calculator
Mounjaro Savings Card and Cost Estimator
If you have any questions regarding insurance coverage or co-pay costs for Ozempic, you can contact Novo Nordisk’s support line at 1-833-OZEMPIC (1-833-693-6742).
For Mounjaro, you can reach out to Eli Lilly’s customer support at 1-800-LillyRx (1-800-545-5979).
Patient assistance programs
For those who qualify, both Novo Nordisk and Eli Lilly offer Patient Assistance Programs (PAP) that provide free or reduced-cost medications. These programs are designed to assist people who do not have insurance or have limited income.
Novo Nordisk PAP (for Ozempic): Call 1-866-310-7549 for more information.
Lilly Cares PAP (for Mounjaro): Call 1-800-LillyRx (1-800-545-5979) for more information.
Always speak with your healthcare provider to understand your eligibility for these programs and to explore any additional savings options.
Can I get off my other diabetes medications if I lose enough weight on Ozempic or Mounjaro?
This is possible but doesn’t usually happen.
Losing weight can help improve both insulin resistance and blood sugar levels. Sometimes this makes your insulin or other diabetes medications unnecessary.
That said, Ozempic and Mounjaro won’t cure diabetes.
However, you may be able to lower your insulin needs or stop taking insulin completely if you’ve lost a significant amount of weight and your blood sugars are very well managed.
This will only apply to people who have type 2 diabetes, as people with type 1 diabetes must take insulin for life.
Check in with your doctor if you have questions about taking your other diabetes medications while on Ozempic or Mounjaro.
Did you find this article helpful? Click Yes or No below to let us know!