As a person living with diabetes, you know it’s important to see your doctor regularly, and that includes seeing a diabetes specialist called an endocrinologist.
The frequency of these types of appointments varies but they usually follow a quarterly hba1c test.
Typically, people with diabetes see their endocrinologist at least once a year for follow-up on management, bloodwork, and to renew prescriptions for medications like Metformin or insulin. To make the most of these appointments, it’s best to be prepared.
This article will outline 10 important questions to ask your endocrinologist the next time you have an appointment.

Table of Contents
- Prep before your appointment
- 10 good questions to ask your endocrinologist
- Is my diabetes in good control for my goals?
- Does the rest of my bloodwork look normal?
- Should I adjust my diabetes medication and/or insulin?
- How can I adjust my care between visits?
- What new insulins, medications and technology is on the horizon?
- Are there any other medications I should be on?
- How can I afford my medications?
- How can I better manage my diet?
- How can I exercise safely and effectively?
- What’s the best thing I can do right now to prevent complications?
Prep before your appointment
Dr. David Lam, Medical Director of the Clinical Diabetes Institute for the Mount Sinai Health System, says, “To get the most from your visit with your endocrinologist, approach it as you might a well-run work meeting.”
Bring a pen and notepad with your personal agenda jotted down before meeting with the doctor, which will outline all of your concerns and any issues you’d like to raise.
“You and the doctor should be on the same page about your main concerns,” Lam says.
It’s also important to bring your blood sugar data from your continuous glucose monitor (CGM) or glucometer with you. Many phone apps can also share this data directly with your endocrinologist’s office.
10 good questions to ask your endocrinologist
Is my diabetes in good control for my goals?
Everyone with diabetes is different, but knowing how your diabetes management stands compared to your goals is very important.
Endocrinologists will usually order bloodwork before an appointment, including the hba1c test, which measures your average blood glucose over the previous 3 months.
Ask your endocrinologist this question directly. Perhaps you’re planning on becoming pregnant in the near future, requiring a much lower hba1c, or maybe you’re trying to figure out why you have a lot of low blood sugars and are aiming to raise your hba1c number a bit.
Whatever your diabetes goal are, make sure they fit your current phase of life.
Does the rest of my bloodwork look normal?
A typical complete laboratory evaluation will measure more than just an hba1c. This thorough blood test measures thyroid functioning, if there’s any protein in the urine, vitamin D levels, cholesterol (HDL and LDL), white and red blood cell counts, and a host of other levels meant to check in on your overall health.
Discuss with your doctor if any of these levels are out of range, especially the markers for Hashimoto’s disease, Antithyroglobulin antibody (TgAb), as well as Tissue Transglutaminase Antibodies (tTG-IgA), a test that will be positive in about 98% of patients with celiac disease.
Both Hashimoto’s and Celiac are common in people with type 1 diabetes.
Should I adjust my diabetes medication and/or insulin?
If you are seeing many high and/or low blood sugars, are struggling with the dawn phenomenon, or are always going high or low after meals or exercise, this is the perfect time to dig deeper into the nitty-gritty of your diabetes management with your endocrinologist.
Based on your most recent blood sugar data, your endocrinologist can help you adjust your correction factor, insulin sensitivity, insulin to carbohydrate ratios, and your basal rates to help fine-tune your management.
This can be especially helpful if you’ve recently changed any lifestyle habits, such as your diet or exercise routine, or are pregnant or planning on becoming pregnant, in which case your hba1c and blood sugar goals may change.
How can I adjust my care between visits?
Seeing the doctor and asking them questions consists of less than 1% of the time you live with your diabetes, and you need to know what to do on the fly if you have an issue.
Say you’re sick and need to vastly increase the amount of insulin you’re taking or training for a marathon and are suddenly extremely insulin sensitive.
This is the ideal time to ask your endocrinologist when and how you can adjust your insulin doses and corrections factors yourself, versus when they would be more comfortable guiding you through any necessary changes.
It’s also helpful to know how available your doctor’s office will be. Can you contact them between visits for quick guidance or advice? Do they answer the phone on weekends? Do they email, text, or use a patient portal? How can you reach them in an emergency?
These are all great questions to ask and something you’ll definitely need to know for optimal care.
What new insulins, medications and technology is on the horizon?
New insulins are constantly hitting the market that work better and faster than even the best available did as little as 5 years ago.
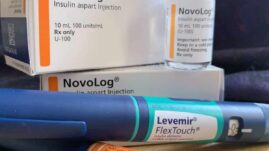
Included among these are Lumjev, Semglee, Tresiba, and Fiasp. Ever hear of them? Ask your endocrinologist about the newest insulins available, and see if they have any free samples that you can try.
In addition to Dexcom’s g7 CGM coming out later this year, patients can look forward to Omnipod’s Horizon system for automated insulin delivery in 2021.
Trying a new type of insulin or the newest technology can mean the difference between out of control blood sugars and an hba1c that you’re truly proud of, but you never know until you try!
Are there any other medications I should be on?
Sometimes insulin isn’t enough. Precision medicine and prescribing medications “off label” is becoming quite popular in the diabetes space.
Sometimes people living with type 1 diabetes will require insulin and metformin to thrive. Other times, a person with type 1 diabetes is prescribed an SGLT2 inhibitor to help manage insulin resistance and weight gain.
Popular drugs for someone with type 1 are Symlin and Victoza – daily injectable prescription drugs that “mimic” the activities of GLP-1, a gut-derived hormone (incretin) that induces insulin secretion from beta cells by binding to GLP receptors in the pancreas.
This helps with satiety after eating, excessive hunger, weight gain, and insulin resistance. Ask your doctor if adding a supplemental prescription drug to your insulin regimen might be right for you.
How can I afford my medications?
The truth is 1 in 4 people with diabetes in the United States rations their insulin due to cost alone. People are struggling and insulin is expensive. A vial of Humalog today costs over $300, whereas when it was introduced to the market in 1996 the same vial cost $21.
If you’re struggling to afford your medications, you’re not alone. Ask your doctor about ways to better afford your medications.
Perhaps you’re eligible for Medicaid in your state, or a tax-subsidized health plan on your state exchange.
Perhaps you’re eligible for reduced or free insulin at a Federally Qualified Health Center that participates in the 340b program.
Perhaps you have a state-regulated health plan that’s subject to a state’s insulin co-pay cap legislation, or perhaps you can seek assistance from a drug manufacturer.
Ask about resources to get the help you need. The help is there, you just have to make your needs known.
How can I better manage my diet?
Diet is a cornerstone of diabetes management, and it’s important to regularly check in on your nutrition. Review your regular diet plan with your doctor, and seek their opinion about any foods that you may need to add or subtract.
Oftentimes a food is delicious, but it isn’t serving you or your diabetes well, and they may know of substitutes that you can try instead.
This is also a good time to mention any issues you may be having with eating, as young people with diabetes are nearly twice as likely to develop an eating disorder as people without diabetes.
If needed, an endocrinologist can write you a referral to see a registered dietitian to better hone your diet, if you’re having trouble with sugar cravings, feeling sated, or are dealing with excess weight gain or fatigue.
How can I exercise safely and effectively?
Exercise is crucial for good diabetes management, but staying motivated isn’t always easy. Talk with your endocrinologist about new exercise ideas for inspiration.
Perhaps you need suggestions on how to winterize your running routine, or are recovering from an overuse injury and need fresh ideas.
You may also be new to exercise, or are struggling with extreme highs or lows from it. Make sure to ask your endocrinologist about how you can better adjust your food intake and insulin for exercise in order to thrive.
According to the Centers for Disease Control and Prevention, adults should aim for 150 minutes of moderate exercise per week, or around 30 minutes most days of the week, so work with your doctor on how to reach at least that amount of exercise every week.
What’s the best thing I can do right now to prevent complications?
If your hba1c and general diabetes management do not align with your goals, it’s time to make an action plan with your doctor. Ask them what you can do today to prevent complications in the future.
Maybe it’s switching up your morning routine to fit in a regular walk, maybe it’s cutting out added sugar on weeknights, or foregoing fast food entirely. Whatever the advice is, make sure you can stick with it and that it will fit into your lifestyle and goals for the long run.
The best time to start preventing diabetes complications is always yesterday. The next best time is now.
Bring these questions and ideas to your next endocrinologist appointment to make the most of your (and the doctor’s) time. Evolved diabetes management starts with asking good questions, so make sure you’re prepared and ready to take charge of your diabetes health!

Stephen
Good list!
Jude Huzicko
I’d be curious to read an article about someone who has both Addison’s and T1D (yes, I know it’s rare.)
Tina Derke
I am a Type 1 diabetic for 34 years. I am so thrilled to have found this newsletter. I have received such valuable info here, more than anywhere else. Each new thing I find out about prompts a discussion with my doctor. Thank you so much. You’ve been a lifesaver.
Melanie Wellington
There is a small error in this article. The idea comes through ok but the actual statement is wrong.
The article says “A typical complete blood count (CBC) test will measure more than just an hba1c. This thorough blood test measures thyroid functioning, if there’s any protein in the urine, vitamin D levels, cholesterol (HDL and LDL), white and red blood cell counts, and a host of other levels meant to check in on your overall health.”
A CBC (complete blood count) measures the levels of blood cells only (Red Blood cells, white blood cells, platelets, etc).
I think it should say “A typical complete laboratory evaluation will measure more than just an HgbA1c….”
Thanks for all the great info – it’s invaluable. I’m only mentioning this to make sure no one reads it and thinks that the CBC test will measure all of those things.
Tobias Oerum
You are absolutely right. Thank you so much for pointing this out. We have updated the article.
Marge
I am prediabetic and have been for over 10 years. My last HbA1C was 6.2, which is my normal range. Do you feel an endocrinologist is necessary. My doctor doesn’t think I need one.
Christel Oerum
That’s a good question. An endocrinologist (who focuses on diabetes) has a deeper knowledge about diabetes than most primary care physicians, so you might get more detailed or different guidance. Your A1C isn’t that high, so you might just be told to keep doing what you’re doing. If you have the means you could always do an initial consult with an endocrinologist and simply ask the person if they would change anything