The “Dawn Phenomenon” or “Dawn Effect” is a term describing when people living with diabetes experience high blood sugar in the morning.
Having your blood sugar rise sharply before you even wake up in the morning can make managing your diabetes more difficult for the rest of the day, so it’s important to identify if you are experiencing Dawn Phenomenon and make a plan for dealing with it.
This article will outline what exactly Dawn Phenomenon is and how to better manage it, so its effects don’t go on to ruin your day.

Table of Contents
- What is the Dawn Phenomenon?
- What causes Dawn Phenomenon?
- What are the symptoms of Dawn Phenomenon?
- How to test for Dawn Phenomenon
- How high a blood sugar is considered Dawn Phenomenon?
- Long term consequences
- How can you manage the Dawn Phenomenon?
- Other reasons for high morning blood sugars
- When to seek care
- Conclusions
What is the Dawn Phenomenon?
Dawn Phenomenon is a condition experienced in people with either type 1 or type 2 diabetes.
It is high blood sugar levels and insulin resistance people experience in the morning, usually between 2 a.m. and 8 a.m.
It usually requires more insulin in the bloodstream during those hours to keep blood sugar levels steady.
Some people need up to double the amount of insulin in their bloodstream overnight to help combat the high blood sugars caused by Dawn Phenomenon.
People without diabetes experience the Dawn Phenomenon as well, but their pancreas increases its insulin secretion to prevent high blood sugars. People with diabetes don’t have that luxury.
It’s estimated that over 50% of people with diabetes suffer from some degree of Dawn Phenomenon!
What causes Dawn Phenomenon?
This biological process dates back to prehistoric times, when humans evolved to have higher blood sugars (and thus more “energy”) in the morning to fuel their hunting and gathering to find food for the day.
The causes of Dawn Phenomenon are mostly hormonal: the natural overnight release of counter-regulatory hormones, such as growth hormone, adrenaline, cortisol, epinephrine, and glucagon increases insulin resistance, resulting in higher blood sugar levels overnight and in the morning.
Additionally, two other processes occur in the liver overnight that result in the release of glucose into the blood, contributing to higher blood sugars:
- Glycogenolysis, which is the breakdown and release of stored glucose
- Gluconeogenesis, which is the creation of glucose from components of protein or fat
Other causes of morning high blood sugar can include insufficient evening mealtime insulin, insufficient insulin basal rates overnight, or even rebound high blood sugars from going low overnight.
It’s important that you don’t blame yourself for experiencing high blood sugar levels from the Dawn Phenomenon!
This is a troubling issue for everyone living with diabetes, and it’s just a matter of figuring out how to best manage and prevent it without blaming yourself or feeling guilty.
“My high sugars in the morning are caused by a combination of dehydration, late-night eating, poor sleep, and hormonal fluctuations.”
Anna Faith (read Anna’s story of managing Dawn Phenomenon)
What are the symptoms of Dawn Phenomenon?
The symptoms of Dawn Phenomenon are the same as having high blood sugar, and they include:
- Fatigue
- Thirst
- Need to urinate
- Headache
- Body ache
- Dry eyes
- Blurry vision
How to test for Dawn Phenomenon
If you notice that you often have high blood sugar in the morning, you can set up a testing routine for a few nights to determine if Dawn Phenomenon is the cause.
To do this, test your blood sugar at the following times:
- before going to bed
- in the early morning, such as between 2:00 a.m. and 4:00 a.m. (set an alarm clock to wake you up)
- as soon as you wake up
If you see that your blood sugar is stable from you go to bed until the early morning and then rises, you are most likely experiencing Dawn Phenomenon.
NOTE: If you have a continuous glucose monitor (CGM), you don’t have to do this test as you can just look at the overnight blood sugar graph it provides.
A blood sugar graph like this is typical for Dawn Phenomenon:
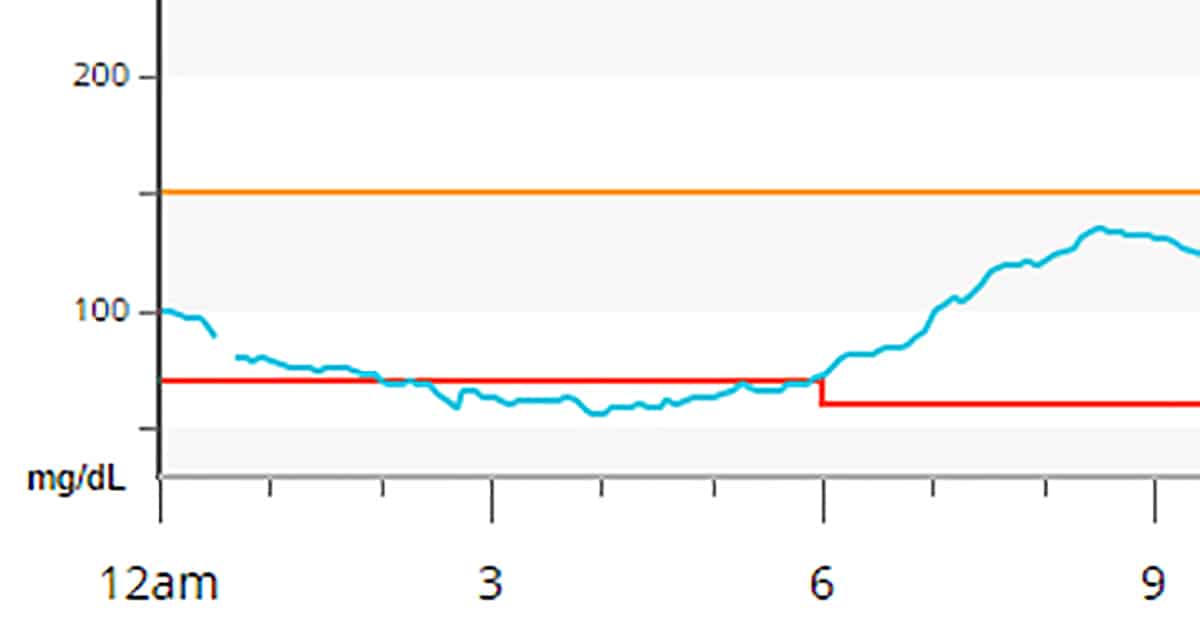
How high a blood sugar is considered Dawn Phenomenon?
Your diabetes experience will vary, but anything higher than is normal for you is considered Dawn Phenomenon.
If you are waking up with higher-than-normal blood sugar levels several mornings a week, it may be time to contact your healthcare provider about readjusting your insulin settings and/or evening routine to help mitigate the issue.
You need to seek help before you experience any long-term damage or complications.
Long term consequences
If left unaddressed, years of experiencing the Dawn Phenomenon and high blood sugars for the majority of the day can result in diabetes complications such as:
- Heart Disease
- Stroke
- Neuropathy, especially in the feet
- Lower leg amputations
- Kidney disease
- Diabetic Retinopathy of the eye
- Premature death
Addressing high blood sugars you may be experiencing while you sleep and into the morning can help prevent and/or delay many (if not most!) of these common complications of diabetes.
How can you manage the Dawn Phenomenon?
Work with your doctor to come up with some solutions that will work to better manage the Dawn Phenomenon you may be experiencing, and always check with your doctor first before adjusting any diabetes medications and/or insulin settings.
Some other strategies may include:
- Avoid lots of carbohydrates or snacks with added sugar at bedtime
- Increasing your protein-to-carbohydrate ratios of evening meals and snacks
- Get plenty of sleep, between 7-8 hours nightly
- Drinking more water in the evening and do not drink liquids with added sugar
- Eat dinner earlier in the evening
- Eat a breakfast lower in carbohydrates, to help manage any higher blood sugars
- Adjust your doses of insulin and/or diabetic medications
- Exercise before bedtime
- Switch from multiple daily injections (MDI) to an insulin pump that can make automatic insulin adjustments while you sleep
- Switch from a regular insulin pump to a hybrid-closed-loop insulin pump, such as the TSlim Control IQ or Omnipod 5
- Change the time at which you take your evening medications
- Split your evening dose of long-acting insulin into two doses (check with your doctor)
- Switch to a different medication that may be more efficacious for you
For a very comprehensive and in-depth guide to managing Dawn Phenomenon if you use insulin, read the article Managing Dawn Phenomenon with Basal Insulin
Other reasons for high morning blood sugars
While Dawn Phenomenon is the most common reason for high morning blood sugar, it’s not the only one. Two other phenomenons can also cause your blood glucose to increase in the morning:
Feet on the floor syndrome
Feet on the flor syndrome is what happens when you wake up with normal blood sugar levels, but as soon as you start moving around in the morning, your blood sugar rises, even without eating anything.
This is usually because your body is releasing counterregulatory hormones, like glucagon and epinephrine, once you’ve started moving around.
Some simple solutions for this may be to increase your morning basal insulin rate, or if you’re not on an insulin pump, to take a small dose of insulin upon waking.
You can learn more about how to manage feet on the floor syndrome in our guide How to Avoid High Morning Blood Sugar
The Samogyi effect
The Samogyi effect also results in high blood sugars upon waking, but for a little bit of a different reason.
if insulin released overnight brings your blood sugars too low, your body will naturally release hormones, such as glucagon and epinephrine, spiking your blood sugar in a rebound high.
This is more common in people with type 1 diabetes than type 2 because everyone with type 1 diabetes takes exogenous insulin and it’s this insulin that is bringing your blood sugar too low overnight.
To counteract this, it can be helpful if you wear a continuous glucose monitor (CGM) and track your blood sugars overnight to see if you’re dipping too low.
Reducing your insulin to carbohydrate ratio at dinner, or lowering your overnight basal rates can help prevent this from happening.
You can learn how to deal with the Samogyi Effect in our guide What is The Samogyi Effect
Other potential causes of high morning blood sugars include but are not limited to:
- any new medications you’re taking
- hormonal changes
- pregnancy
- insulin resistance
- a failed insulin pump and/or CGM site
- stress
- lack of sleep
- a miscalculation of an evening bolus
Christel Oerum, who lives with type 1 diabetes, has recorded a great YouTube video where she gives her best tips for preventing high morning blood sugars. It’s well worth watching:
When to seek care
High morning blood sugars are not more dangerous than high blood sugars at other times of the day, so you don’t need urgent care because you experience Dawn Phenomenon.
However, because Dawn Phenomenon can be a persistent issue, it can lead to long-term diabetes complications.
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) therefore recommends that you see your doctor or endocrinologist if your morning blood sugar is high more than three times in a 2-week period.
Your doctor can help you determine if you are experiencing Dawn Phenomenon and suggest changes to your lifestyle, medication, and diabetes management.
Conclusions
Everyone in the world experiences the Dawn Phenomenon, but people with insulin-dependent diabetes are most susceptible to the insulin resistance and stubborn high blood sugars that result from this natural, hormonal occurrence.
It is nothing to feel guilty about, nor be ashamed about, but by taking proactive steps, you can help mitigate, manage, and even prevent the Dawn Phenomenon from ruining your day and diabetes management.
The Dawn Phenomenon can be dangerous if experienced long-term, leading to diabetes complications.
Be sure to implement prevention strategies, such as incorporating evening exercise, limiting carbohydrates at dinner, and increasing your protein-to-carbohydrate ratios, if you’re regularly struggling with the Dawn Phenomenon.
Always work with your doctor first before adjusting any basal/bolus insulin settings (if you’re on an insulin pump), splitting your evening dose of long-acting insulin, or increasing your insulin doses.



Ann
I’m not able to regulate my BG at anytime of day. I’m a very brittle type one I can’t seem to ever get a rhythm of numbers that make sense but it goes from high to low even though I eat very clean.
I’ve been recommended to get a diabetic alert dog. I’ve been having such issues trying to find a reputable placement organization. The international assistance organization doesn’t have any local resources for Connecticut.
Any help is so greatly appreciated sincerely yours.
Christel Oerum
This is the only resource we have on how to get a diabetes alert dog: https://diabetesstrong.com/how-to-get-a-diabetes-alert-dog/
Mason Taylor
Yes, I evenly split my long-acting insulin (Lantus brand of glargine): 6 units at about 6 am and 6 units at about 6 pm. (I’ve heard some divide long-acting into 3 doses/day.)
Intuitively this makes more sense than one large dose per day.
Nevertheless, my Dexcom today typically started alerting me at 4 AM my bg had fallen to 68. I ignored it and turned over. By 5:30 AM my bg was slowly rising and continued till I took 0.5 units fast-acting at 5:50 AM, then did my breathing and some stretching exercises.
By 6:23 am, my bg was 72 mg/dL and I injected my morning long-acting glargine, prepared breakfast, did some more asanas.
By 6:38 am bg had risen a little more, I injected remaining 5 units fast-acting (Humalog brand lispro) and then ate breakfast. At 9:41 am (2-hour postprandial) my bg is an acceptable 125 mg/dL.
Thanks again for a fact-filled very helpful article. I welcome any feedback.
Christel Oerum
What I like about your strategy is, that it’s based on experience and, clearly, paying attention to how your body fluctuates with your hormones. I’ll often do as you do about a 5-6 AM low-ish alarm or only take 0.5-1 glucose tab. I don’t want to go lower than 6.8/70 mg/dL, even if I know it will start to climb, I’ll still nibble on a glucose tablet